Syphilis as the cause of disseminated ulcerated crusted skin lesions in an immunosuppressed patient
DOI:
https://doi.org/10.5935/2764-734X.e202205011Keywords:
Syphilis, Cutaneous, Acquired Immunodeficiency Syndrome, Warts, Case ReportAbstract
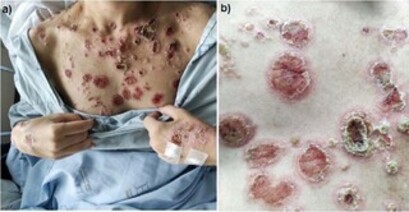
Individuals infected with the human immunodeficiency virus (HIV) have a higher risk of co-infection with syphilis, and may have a different course of evolution from those who are seronegative, sometimes faster and more aggressively. The manifestation of secondary syphilis is proportionately more prevalent, with malignant syphilis (MS) being a rare form of this stage of the disease, but with a significant increase in the number of cases after the AIDS epidemic. MS presents with pleomorphic lesions, classically described as disseminated ulcero-nodular lesions, accompanied by more intense constitutional symptoms. This report describes the case of a female patient whose diagnosis of HIV was simultaneously established with that of recent syphilis, which occurred during the investigation of disseminated, ulcerated and crusted skin lesions, sometimes with a rupioid appearance. The diagnosis of secondary syphilis was established in association with asymptomatic neurosyphilis. Despite the clinical and laboratory criteria compatible with the diagnosis of MS, the infrequent cutaneous presentation deserved the differential diagnoses grouped as a verrucous syndrome, especially sporotrichosis.
Downloads
References
1. Ghanem KG, Ram S, Rice PA. The Modern Epidemic of Syphilis. N Engl J Med. 2020; 382(9):845-854.
2. Karp G, Schlaeffer F, Jotkowitz A, Riesenberg K. Syphilis and HIV co-infection. Eur J Intern Med. 2009; 20(1):9-13.
3. Zetola NM, Klausner JD. Syphilis and HIV infection: an update. Clin Infect Dis. 2007; 44(9):1222-8.
4. Cid PM, Cudós ES, Zamora Vargas FX, Merino MJ, Pinto PH. Pathologically confirmed malignant syphilis using immunohistochemical staining: report of 3 cases and review of the literature. Sex Transm Dis. 2014; 41(2):94-7.
5. Wibisono O, Idrus I, Djawad K. Sífilis maligna: revisión sistemática de los casos publicados entre los anos 2014-2018. Actas Dermosifiliogr. 2021; 112:725-734.
6. Fisher DA, Chang LW, Tuffanelli DL. Lues maligna: presentation of a case and a review of the literature. Arch Dermatol. 1969; 99(1):70-3.
7. Gregory N, Sanchez M, Buchness MR. The spectrum of syphilis in patients with human immunodeficiency virus infection. J Am Acad Dermatol. 1990; 22:1061-7.
8. Sands M, Markus A. Lues maligna, or ulceronodular syphilis, in a man infected with human immunodeficiency virus: case report and review. Clin Infect Dis. 1995; 20:387-90.
9. Costa PP, Moura AA, Rodrigues FLM, Almeida MP, Vilasboas V, Francesconi F. Sífilis maligna precoce em paciente imunodeprimido. Revista SPDV 2019; 77(2).
10. Rosenheim M, Brucker G, Leibowitch M, Niel G, Bournerias I, Duflo B, et al. Syphilis maligne chez un malade porteur d’anticorps anti-HIV [FRE]. Presse Med. 1987; 16(16):777.
11. Santos TR, Castro IJ, Dahia MM, Azevedo MC, Silva GA, Motta RN, et al. Malignant syphilis in an AIDS patient. Infection. 2015; 43(2):231-6.
12. Costa F, Martinez C, Azulay L. PLECT: enfermedades tropicales de manifestación verrucosa. Rev chil dermatol. 2018; 34(3):89-94.
13. Marra CM, Maxwell CL, Smith SL, Lukehart SA, Rompalo AM, Eaton M,et al. Cerebrospinal fluid abnormalities in patients with syphilis: association with clinical and laboratory features. J Infect Dis. 2004; 189:369-76.
14. Libois A, De Wit S, Poll B, Garcia F, Florence E, Del Rio A, et al. HIV and syphilis: when to perform a lumbar puncture. Sex Transm Dis. 2007; 34(3):141-4.
15. Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Departamento de Vigilância, Prevenção e Controle das Infecções Sexualmente Transmissíveis, do HIV/Aids e das Hepatites Virais. Protocolo clínico e diretrizes terapêuticas para manejo da infecção pelo HIV em adultos. Brasília: MS; 2018.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2022 Infections in Evidence

This work is licensed under a Creative Commons Attribution 4.0 International License.
All users may freely read, download, share, and adapt this scientific product for any purpose (even commercial ones), provided that due credit is given to the authors and the original publication, and that any alterations are duly indicated.
> Ethics
All articles published herein have received ethical approval from the National Research Ethics System (formerly CEP/CONEP system) based on Federal Law 14.874/24 and other specific Brazilian regulations, or a similar document attesting to the knowledge and authorization from the institution of origin in the case of foreign works.
The authors declare that there is no sponsorship or conflict of interest of any kind, unless otherwise indicated in the body of the article.
It is worth noting that case reports are a valuable learning resource for the scientific community, but should not be used in isolation to guide diagnostic or therapeutic options in clinical practice or health policies
















